Diabetic Retinopathy (DR)
Retina is the light sensitive film in the back of the eye on which the rays of light are brought to focus to form an image. This image is transmitted to the brain by the optic nerve. The vitreous is the clear gel that fills the back of the eye. The “Macula” is the central portion of the retina that is responsible for the most of our vision.
Diabetes causes weakening of the blood vessels in the body including those of the retina. This deterioration of retinal blood vessels, accompanied by structural changes in the retina, is termed diabetic retinopathy and in the severe stage may lead to loss of vision. Diabetic retinopathy occurs in more than half of the people who develop diabetes. The condition can develop in anyone who has type 1 or type 2 diabetes.
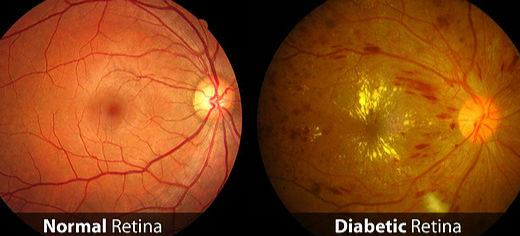
Types of DR
There are two main forms of diabetic retinopathy. The first is the non-proliferative type, or background retinopathy. The second type is proliferative retinopathy. The non-proliferative type, is usually less severe. This type is a warning sign to the possible progression to proliferative retinopathy.
Macular edema can degrade the critical central vision. The area of the macula can thicken, as fluid from leaking blood vessels pools within the retinal layers. In addition to these fluid pockets, the important retinal neurons critical to central vision can be damaged or lost.
Laser may be applied around the macula to reduce fluid leakage as a treatment of macular edema.
New treatment approaches exist for some types of macular edema and the wet form of macular degeneration. Angiogenesis inhibitor medications known as Anti-VEGF, are injected into the eye. They look to inhibit the growth of new blood vessels and neovascular tissue. However, unfortunately, it will not restore vision that is already lost.
Symptoms
1. Spots or dark strings floating in your vision (floaters)
2. Blurred vision
3. Fluctuating vision
4. Impaired colour vision
5. Dark or empty areas in your vision
6. Vision loss
7. Diabetic retinopathy usually affects both eyes
Risk factors
All types of diabetic patients are at risk for diabetic retinopathy. Risk increases the longer a person has diabetes.
Diagnosis
1. Visual acuity testing: Eye chart to measure near and distance vision
2. Tonometry: This test measures pressure inside the eye.
3. Pupil dilation: Instil drops in eyes to widen or dilate the pupils to view back of eye
4. Optical coherence tomography (OCT): capture images of tissues inside the body. OCT provides detailed images of tissues that can be penetrated by light, such as the eye.
5. Fluorescein angiogram: may be used to look for damaged or leaky blood vessels.
DR can be prevented
1. Early treatment can reduce risk of blindness by 95%. It is recommended that people with diabetes should get dilated eye exam once in year
2.Optimal glucose control reduces the risk of DR
Treatment
1. Anti-VEGF Injection
2. Focal/grid macular laser
3. Corticosteroids
4. Pan retinal Photocoagulation
5. Vitrectomy
Summary
Those with diabetes should have frequent eye exams. Early detection is very important to management of diabetic retinopathy. Treatments may halt, slow, or in some cases, fail to control the progression of this very serious and difficult eye disease. Any changes to your vision should be brought to your eye care provider’s attention immediately.
Contact Us
If you have any other questions or concerns, please contact us at:
The Eye clinic
Dr Swati Agarwal -The Eye Clinic
2A Motilal Basak lane
Kakurgachi
Kolkata, WB 700054
www.swatiagarwal.in
+91 9147714355
[email protected]
Important Note
This information is provided for general educational concepts only. Your specific circumstances, conditions, treatment approaches, and results may vary from those shown here. Additional information, instructions, and precautions are to be provided by and discussed with your eye care provider.
Need Urgent Help?
Call Us: